From a longevity perspective, optimizing metabolic health is one of the most important things to do because metabolic disease is a major driver of the three diseases that are killing about 80% of people in the West:
If my metabolic state is bad, this is going to increase the risk for each of these three plagues of modern civilization.
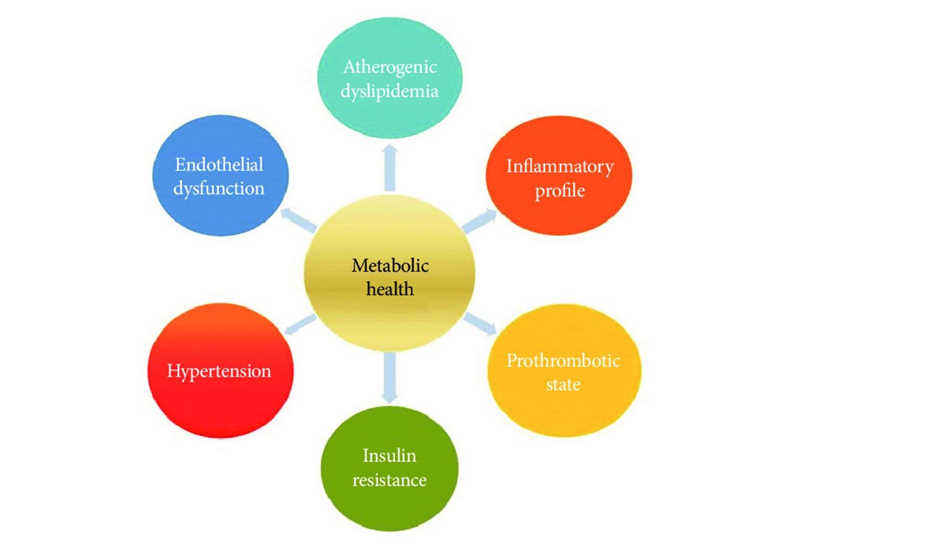
What is metabolic health exactly?
In short, metabolic health determines how capable my body is at partitioning and using energy. Ideal metabolic health would include good insulin sensitivity, great metabolic flexibility, and adequate nutrient partitioning. I will briefly discuss all three of them.
- High insulin sensitivity allows for blood glucose levels to be kept normal with only small amounts of insulin (insulin is discussed in detail here). In general, high fasting levels of insulin (a potent growth factor) drive the mTOR pathway, which then drives cellular senescence, adiposity, inflammation, atherosclerosis, tumorigenesis, and neurodegeneration.
- Metabolic flexibility means that my cells have no issue switching from burning glucose to burning fatty acids for energy, and vice versa. However, they need to be trained to do so, for example, via endurance exercise, smart dietary choices, reducing body fat levels, or taking metabolic drugs.
- Adequate nutrient partitioning means that energy is predominantly used for fuel, and any surplus of glucose and fatty acids is swiftly taken up and used by non-fat cells instead of being stored as fat in visceral adipocytes, God forbid, non-fat cells.
One can gauge one’s own metabolic status by taking into account several blood markers (e.g., HBA1C, CRP, fasting insulin), insulin sensitivity (e.g., measured via OGTT or CGMs), and body fat percentage.
What causes metabolic disease?
Metabolic derangement is an incredibly complex issue, particularly because a number of things are happening in parallel and are interacting with each other in complex feed-back and feed-forward loops.
Just as many roads lead to Rome, metabolic disease can start with a handful of different things, including prolonged hyperinsulinemia for whatever reason, prolonged hypercortisolemia for whatever reason, systemic inflammation, or visceral adiposity.
Furthermore, there are a large number of more and less important players that are all either promoting or impairing metabolic health. Some of these factors include the activity of mTOR or AMPK (regulators of intracellular metabolism), hundreds of genetic factors, about a dozen hormones or cytokines (inflammatory mediators).
Many factors are deeply intertwined, and it is nearly impossible to determine what causes what and how these factors interact. Nonetheless, the Tiber (the big river to which many other rivers converge) is “insulin all of the time” (hyperinsulinemia). I discuss insulin in more detail here: Insulin, Insulin Resistance, and Strategies I Use to Keep High Insulin-Sensitivity Year-Round
To become metabolically healthy, the Tiber needs to be drained. While many things can be done, the most effective ways to drain the Tiber and to reclaim land are, in my opinion, getting rid of visceral fat, gaining muscle mass, endurance exercise, avoiding spikes in blood sugar, optimizing sleep, managing stress, and optimizing hormones. Metabolic drugs can also be very useful (as discussed later).
These six pillars also have huge preventative power and keep metabolic health from deranging.
I will briefly discuss each of them.
How to improve metabolic health: The Seven Pillars
Pillar #1: Getting rid of visceral fat
Visceral adiposity in general leads to a fatty liver, which wreaks havoc on all aspects of metabolic health, particularly insulin sensitivity. The science is quite complex and has to do with local adipokine signaling, local elevation of free fatty acids activating the inflammasome, and free fatty acids inducing physiological insulin resistance.
While visceral fat is a driver of insulin resistance, it is also a consequence of it (remember: many things are happening in parallel).
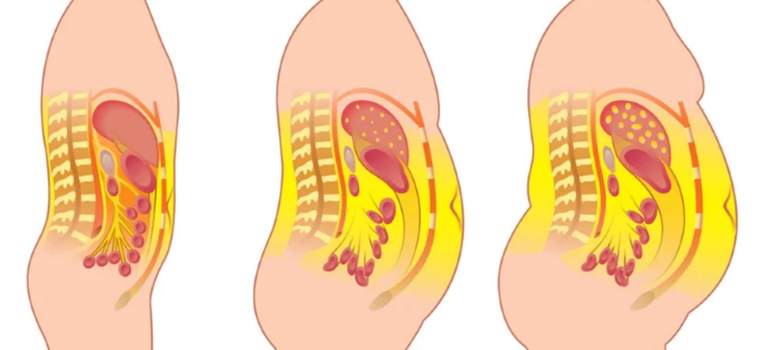
What can be done about it?
#1 Losing body fat
In general, visceral adiposity correlates fairly well with body-fat percentage, particularly in men (testosterone is lipolytic to subcutaneous fat) while premenopausal women are somewhat protected (estradiol primes the body to store fat subcutaneously). If body fat is lost, visceral fat will be lost as well.
Losing excess fat is presumably the most efficient and effective way to reduce visceral fat. This can be done via the old school “diet & exercise” way, hormone optimization, or pharmacologically via e.g., GLP-1 agonists such as semaglutide. I discuss this in more detail here: Why Weight Loss is Not About “Calories In vs. Calories Out”
#2 Cutting out sugar and alcohol
Fructose overconsumption can specifically induce visceral fat accumulation. Fructose restriction is a powerful tool to reverse NAFLD because fructose is metabolized differently than glucose (as discussed here). The same holds for ethanol, which is basically “fructose without the buzz”.
#3 Managing stress and optimizing sleep
Both stress and sleep deprivation increase levels of cortisol. Cortisol affects trunk vs. peripheral adipocytes differently. In the periphery, cortisol is lipolytic, while in the trunk, cortisol is obesogenic. Therefore, stress reduction and sleeping well help.
#4 Reducing AUC levels of insulin:
The most effective way to lower insulin is to not eat. However, multiple-day fasting can have many downsides (I share my experience with it here.) Two other ways to lower area-under-curve insulin levels are low-carb diets, intermittent fasting, or a ketogenic diet.
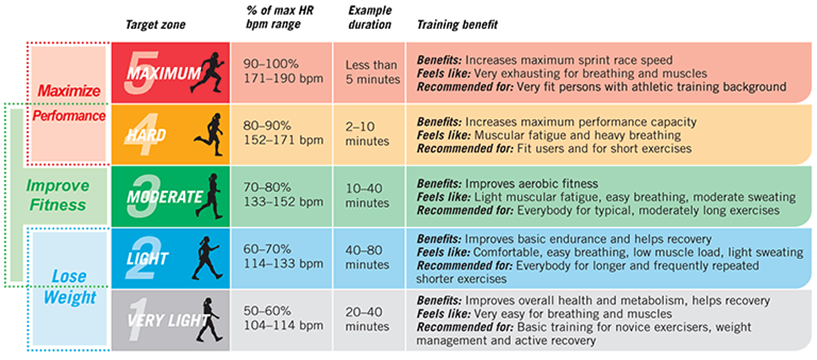
Pillar #2: Having a good VO2 max
Exercise, in particular endurance exercise, leads to countless adaptations in skeletal muscle. One of the presumably most important changes is an improvement in mitochondrial function and a stimulation of mitochondrial biogenesis.
Furthermore, endurance exercise stimulates an insulin-independent GLUT-4 translocation, which will reduce blood glucose levels in an insulin-independent way. Moreover, endurance exercise also leads to a depletion of intracellular nutrient stores (particularly glycogen), which activates AMPK.
On an epigenetic level, endurance exercise also leads to altered expression of a large number of genes.
Because of these changes, a single endurance exercise session increases insulin sensitivity for the next 24 hours or so. By regularly depleting glycogen stores, dietary glucose is handled the way it should be, namely, by being funneled into hepatic or muscle glycogen synthesis. Conversely, if glycogen stores are always tapped out, excess glucose is biochemically much harder to manage and comes with a host of unfavorable biochemical alterations.
Pillar #3: Having a decent amount of muscle mass
Muscle tissue is relatively metabolically active at rest and the more muscle mass someone has, the more glucose and fatty acids are mopped up by muscle tissue, which increases insulin sensitivity because muscle acts as a “glucose sink”.
Muscle mass is acquired by progressive overload and an adequate caloric intake. Obviously, “never skip leg” because legs have by far the biggest muscle groups in the body. I discuss my approach to building and maintaining muscle mass in more detail here.

Having a decent amount of muscle mass will improve any aspect of metabolic health discussed above: insulin sensitivity, nutrient partitioning, and metabolic flexibility.
Pillar #4: Optimizing sleep
There are multiple ways in which bad sleep hampers metabolic health.
- In a sleep-deprived state, cortisol levels are generally high. Cortisol has a huge effect on various aspects of metabolism.
- Good sleep is necessary for proper growth hormone release. Growth hormone is anabolic to muscle and catabolic to fat, particularly visceral fat (discussed shortly).
- The nervous system itself is quite a powerful regulator of metabolic status. For example, through vagal nerve endings, the nervous system affects liver metabolism and insulin secretion. Bad sleep is usually associated with greater basal insulin secretion, likely independent of cortisol and presumably mediated by vagal control of the pancreas.
- In a sleep-deprived state, willpower and metacognition are poor, which leads to bad food choices and forgoing exercise, both of which are causally related to metabolic health.

I discuss how I optimize my sleep in more detail here.
Pillar #5: Stress management
It is widely recognized that diabetes mellitus is more prevalent among people who have a stressful lifestyle. There are two major reasons for this.
Firstly, stress makes it hard to live a healthy lifestyle. When stressed, many people make worse food choices or have trouble managing their sleep. Furthermore, a stressful lifestyle is usually associated with less time (or will) to exercise.
Secondly, people who are stressed will secrete higher amounts of cortisol. People with Cushing syndrome (cortisol excess) almost always have metabolic syndrome (high blood pressure, high blood lipids, high blood sugar). Cortisol is a powerful steroid hormone, which directly or indirectly affects about 10-20% of the human genome. I discuss cortisol in more detail here.
When cortisol levels are high, visceral adiposity increases, insulin resistance increases, blood glucose is higher, and many genes are altered in an “anti-longevity” way.
Every person has their own means to alleviate stress. These may include meditation, exercise, mindfulness, playtime, sex, socialization, or antidepressants.
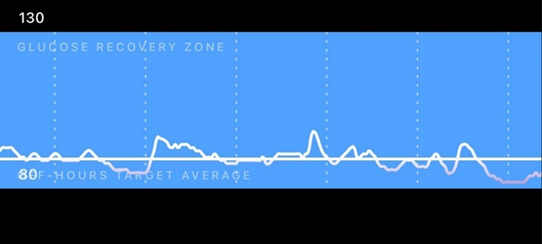
Pillar #6: Avoiding spikes in blood sugar
With a few exceptions, blood sugar spikes essentially come down to eating starchy food low in fiber or consuming sugary crap (e.g., sweets, soft drinks).
Generally, avoiding unnatural spikes in insulin is “better” for a variety of reasons. Insulin is the master control hormone of metabolism and turns a lot of metabolic gears in an unfavorable way. I discuss insulin in much more detail here.
Pillar #7: Hormone optimization
If one of the major hormones is off, metabolic health is much harder to attain, even if all of the other factors are taken care of. Furthermore, if one of the major hormones is low, people often lack the energy and mood necessary to take care of the other pillars.
In my biochemistry classes, I learned a whole lot about intracellular energy metabolism, though for the most part, my professors never really did a good job at explaining that hormones have the power to override much of what is decided at the cellular level in order to coordinate metabolism on a body-wide level depending on specific circumstances (e.g., growth, abundance, stress, pregnancy, starvation, etc.).

There are over 30 hormones that regulate metabolism in one way or another. Many of these hormones have a say in what happens to the calories I ingest. However, different hormones are of different importance and also do different things.
For example (and very simplistically speaking):
- Thyroid hormones: Thyroid hormones regulate “metabolic speed”. Thyroid hormones increase the general rate at which metabolic processes are happening and therefore their effects can either be anabolic or catabolic, depending on caloric intake and the presence of anabolic hormones. In general, having good thyroid function improves blood pressure, blood sugar, and blood lipids. Unfortunately, many physicians reach for a plethora of drugs to manage these instead of ever looking at thyroid hormone function. I discuss my experience with thyroid hormones in more detail here.
- Cortisol: As their name suggests, stress hormones prepare the body for stress. In humans, cortisol is the primary stress hormone. Cortisol stimulates gluconeogenesis & lipolysis and downregulates protein synthesis. Unfortunately, bringing down cortisol levels is hard. Some people have some success with adaptogens (ashwagandha and rhodiola) or phosphatidylserine. Others have success with optimizing sleep or meditation.
- Sex hormones: Sex hormones regulate nutrient partitioning. Among other things, testosterone is anabolic to muscle and catabolic to subcutaneous fat, while estradiol stimulates the deposition of subcutaneous fat (presumably to prepare the organism for pregnancy). I discuss my experience with testosterone in more detail here.
- Leptin: Leptin prepares the organism for starvation. In its absence, the synthesis of other hormones (except for cortisol) is vastly reduced. Furthermore, what is not known to many, leptin directly regulates the metabolism of the liver, muscle, and fat (which comprise about 80% or so of body mass). I discuss my experience with leptin in more detail here.
- GH: Growth hormone is catabolic to adipose tissue and anabolic to everything else. Growth hormone is particularly powerful in reversing a fatty liver, as it is highly lipolytic to visceral fat. GH also stimulates the synthesis of IGF-1, which is anabolic to everything. I discuss GH & IGF-1 in more detail here.
Then there is insulin, which is the most important metabolism-regulating hormone of all. I discuss insulin and insulin resistance in more detail here: Insulin & Strategies I Use To Keep Insulin Sensitivity High Year-Round

Ranking
My personal intuition about how these pillars may be ranked:
- #1: Getting rid of visceral fat
- #2: Training VO2 max & having a decent amount of muscle mass
- #4: Metabolic drugs
- #5: Optimizing sleep
- #6: Managing stress
- #7: Avoiding spikes in blood sugar
Bonus: Taking metabolic drugs
Even though not necessarily necessary, metabolic drugs can have a fairly big impact on metabolic health. Metabolic drugs are as much an (inadequate) “replacement” for the pillars outlined above as they can be used to improve things even more.
Metabolic drugs include metformin, acarbose, allopurinol, SGLT-2 inhibitors, rapamycin, and GLP-1 agonists. I discuss these, and my experience with them, in more detail here: Metabolic Drugs
My own approach to metabolic health
I discuss the specific strategies I follow to ensure good metabolic health in detail here.
Sources & further information
- Molecular mechanisms linking stress and insulin resistance
- The acute vs. chronic effect of exercise on insulin sensitivity: nothing lasts forever
- Study of Insulin Resistance in Subclinical Hypothyroidism
Disclaimer
The content available on this website is based on the author’s individual research, opinions, and personal experiences. It is intended solely for informational and entertainment purposes and does not constitute medical advice. The author does not endorse the use of supplements, pharmaceutical drugs, or hormones without the direct oversight of a qualified physician. People should never disregard professional medical advice or delay in seeking it because of something they have read on the internet.
